Share this post:
Author: Zachary R. Noel, PharmD, BCPS
Given the extensive role that platelet activation and aggregation play in the pathophysiology of acute coronary syndromes (ACS), it seems reasonable to administer a P2Y12 inhibitor, in combination with aspirin and an anticoagulant (e.g., heparin or enoxaparin), as early as possible to minimize thrombus formation and progression of ischemia. Nonetheless, there remains considerable controversy surrounding the optimal timing of P2Y12 inhibitor administration in those undergoing percutaneous coronary intervention (PCI), particularly those presenting with non-ST-segment-elevation acute coronary syndrome (NSTE-ACS). One of the proposed disadvantages of early, upfront P2Y12 inhibitor administration prior to PCI (also referred to as “upstream” administration) is that patients who may derive greater benefit from coronary artery bypass graft (CABG) surgery based upon angiographic findings would then require a P2Y12 inhibitor washout period before surgery to ameliorate bleeding risks (TABLE 1). In theory, this equates to increased length-of-stay, hospital-related complications, and patient dissatisfaction. For these reasons, some practitioners prefer to administer P2Y12 inhibitors on a provisional basis after the coronary anatomy has been characterized by angiography (also referred to as “downstream” administration).
TABLE 1
| P2Y12 inhibitor | Recommended Washout Period to Minimize CABG-Related Bleeding1 |
| Clopidogrel | 5 days |
| Prasugrel | 7 days |
| Ticagrelor | 5 days |
Although the potential to delay CABG and prolong hospitalizations may be an undesired consequence of early P2Y12 inhibitor administration in NSTE-ACS, the data are unclear that delayed administration confers improvements in outcomes or reduces the time to CABG. In this blog, we’ll briefly explore some of the data for upstream administration of P2Y12 inhibitors in NSTE-ACS and how this approach may impact those patients requiring CABG.
Potential Benefits of Upstream P2Y12 Inhibitor Administration
To validate the temporal relationship of P2Y12 inhibitor administration and clinical outcomes, one need look no further than the landmark trial of clopidogrel in ACS, the Clopidogrel in Unstable Angina to Prevent Recurrent Events (CURE) trial.2 In CURE, patients were randomized to aspirin or aspirin plus clopidogrel within 24 hours of presentation for NSTE-ACS. The primary endpoint, composite death from cardiovascular causes, nonfatal stroke, and nonfatal myocardial infarction, was significantly lower in those treated with clopidogrel (11.4% v 9.3%; RR 0.80; p<0.001) and was observed within days of randomization. Although only ~20% of patients received PCI in CURE, this subgroup showed consistent benefit when treated with clopidogrel before PCI.3 Those treated with clopidogrel had fewer myocardial infarctions prior to PCI (5.1% v 3.6%; RR 0.68; p=0.04), as well as fewer combined cardiovascular death and myocardial infarction before and after PCI (12.6% v 8.8%; RR 0.69; p=0.002). Although these results favor early P2Y12 inhibitor administration, it should be noted that the median time to PCI was 10 days and thus these findings may not be generalizable to current practice, which generally consists of earlier invasive strategies.
The results from the Trial to Assess Improvement in Therapeutic Outcomes by Optimizing Platelet Inhibition with Prasugrel (TRITON– TIMI 38) provide additional evidence for an upstream approach, particularly since the trial’s design is more consistent with current practices.4 TRITON-TIMI 38 enrolled patients presenting predominantly with NSTE-ASC who planned to undergo a primary invasive treatment approach. Patients were randomized to either clopidogrel 300 mg or prasugrel 60 mg, which was administered during PCI in 75% of the patients enrolled. Although prasugrel fared better compared to clopidogrel with respect to composite death from cardiovascular causes, nonfatal MI, or nonfatal stroke over the 14 months of follow-up, the effects were most recognizable within the first day of randomization (Figure 1). The most likely explanation for this finding is the suboptimal clopidogrel loading dose used. Clopidogrel 300 mg achieves only 40% inhibition of platelet aggregation at its peak effect, which occurs ~4 hours after administration.5 When the dose is increased to 600 mg, inhibition of platelet aggregation is increased to 60% within 2 hours of administration. Prasugrel 60mg, on the other hand, produces 80% inhibition of platelet aggregation within 1-2 hours of administration. This raises the question as to whether prasugrel would have still shown an improvement had clopidogrel been loaded with 600 mg prior to PCI.
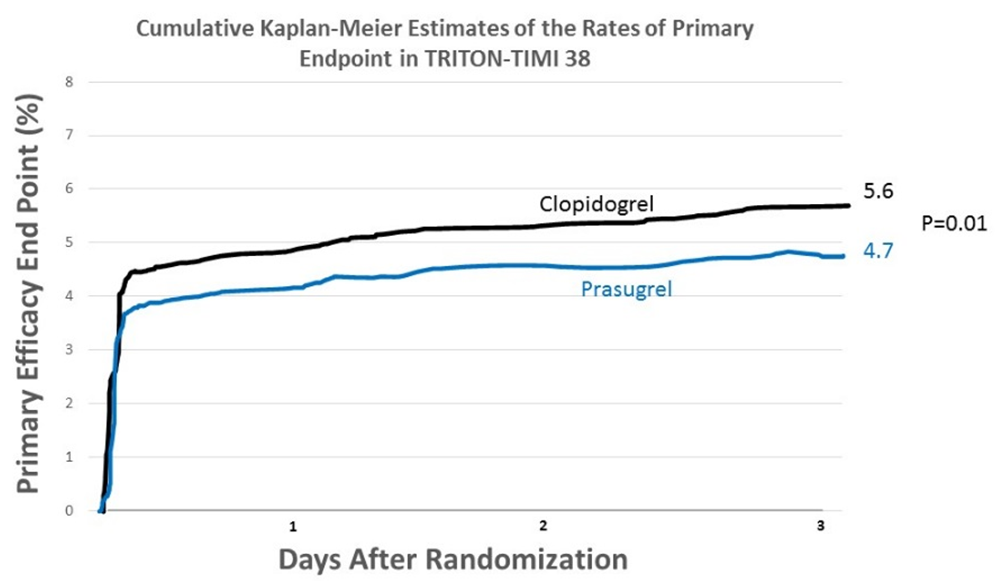
Adapted from TRITON-TIMI 38 trial.4
Also supporting an upstream approach are the results from the Study of Platelet Inhibition and Patient Outcomes (PLATO), which compared ticagrelor to clopidogrel in patients presenting with ACS.6 Approximately 60% of the patients in PLATO presented with NSTE-ACS, and of those the average time from administration of ticagrelor or clopidogrel to PCI was 3.93 and 3.65 hours, respectively. Although the upstream doses of clopidogrel were only 300 mg, an additional 300 mg was administered if PCI was performed. Ticagrelor showed an overall improvement in the primary outcome of composite death from cardiovascular cause, MI, and stroke (9.8% v 11.7%; p-value < 0.001) as well as a mortality benefit (4.5% v 5.9%; p-value < 0.001). Although PLATO did not compare upstream vs. downstream P2Y12 inhibitor administration strategies per se, it is important to note the timing of ticagrelor administration and recognize that we do not have data to suggest alternative timing is better.
It should be noted that, although there are potential benefits of upstream P2Y12 inhibitor administration, the data are conflicting. Current guidelines do not provide meaningful recommendations on this issue. One of the few trials evaluating upstream vs. downstream administration – and perhaps the most relevant for this discussion – is the Comparison of Prasugrel at the Time of Percutaneous Coronary Intervention (PCI) or as Pretreatment at the Time of Diagnosis in Patients with Non-ST Elevation Myocardial Infarction (ACCOAST) trial.7 This trial compared upstream prasugrel with provisional prasugrel after coronary angiography, and found no reduction in the composite endpoint of death from cardiovascular causes, MI, stroke, urgent revascularization, or rescue glycoprotein IIb/IIIa inhibitor at 7 days. Those pretreated with prasugrel did, however, have increased composite CABG-related and non-CABG-related TIMI major bleeding (2.6% v 1.4%; p-value 0.006). Although this trial showed upstream administration with prasugrel produced more harm than benefit, it is important to not extrapolate this data to other P2Y12 inhibitors, which have different pharmacokinetic profiles and baseline rates of bleeding events.
The CABG Quandary
There also remains concern by some practitioners that an upstream approach may interfere with patients receiving in-hospital CABG in a timely fashion. Although these concerns are valid, the percentage of patients admitted for NSTE-ACS who undergo in-hospital CABG is quite small. Recent observational data has shown that only 10% of patients hospitalized for NSTE-ACS will have in-hospital CABG, and of those less than half will have surgery within 72 hours of presentation.8-11 In addition, initial P2Y12 inhibitor selection could significantly impact the necessary washout period and time to CABG. As previously mentioned, clopidogrel and prasugrel warrant a longer washout period due to their irreversible activity on P2Y12 receptors. On the contrary, ticagrelor is a reversible inhibitor and has a relatively short half-life (~7 hours for ticagrelor and ~9 hours for its active metabolite).12 Large cohort studies have shown the greatest risk for CABG-related bleeding appears to be in those who receive ticagrelor within 24 hours of CABG; however, contrary to current package-label recommendations, those who receive it 24-72 hours prior to CABG do not appear to be at an increased risk for bleeding complications.13-14 Perhaps the rapid onset (and offset) and more complete platelet inhibition afforded by ticagrelor make it a more preferred option for early, upstream administration in NSTE-ACS.
Bottom Line: Although there are not clear data on the benefits of upstream administration of clopidogrel or ticagrelor in NSTE-ACS, there is anecdotal evidence that it could be advantageous. The Downstream Versus Upstream Strategy for the Administration of P2Y12 Receptor Blockers (DUBIUS) trial is ongoing and will hopefully provide clarity on the optimal timing of P2Y12 inhibitor administration. Until then, providers should recognize the low likelihood that a patient will need in-hospital CABG (i.e. <5-10%) and weigh it against the potential benefits of upstream P2Y12 inhibitor administration.
Take home points:
- Current guidelines do not provide specific recommendations for timing of P2Y12 inhibitor administration, with the exception of upstream prasugrel, which should be avoided based on results of the ACCOAST trial.1,7,15
- It is reasonable to consider ticagrelor as an “empiric” upstream P2Y12 inhibitor of choice in patients presenting with NSTE-ACS given its favorable pharmacokinetic profile. Should CABG be warranted, the delay in surgery could potentially be minimized (i.e., as little as 72 hours) as compared to clopidogrel or prasugrel.
For additional readings on the timing of P2Y12 inhibitor administration, please see the following links:
- Pretreatment With P2Y12 Inhibitors in Non–ST-Segment–Elevation Acute Coronary Syndrome Is Clinically Justified
- Pretreatment with P2Y12 Inhibitors in Non–ST-Segment–Elevation Acute Coronary Syndrome: An Outdated and Harmful Strategy
 |
Zachary R. Noel, PharmD, BCPS
|
References
- 2015 ESC Guidelines for the Management of Acute Coronary Syndromes in Patients Presenting Without Persistent ST-Segment Elevation. European Heart Journal (2016) 37, 267–315
- Effects of Clopidogrel in Addition to Aspirin in Patients with Acute Coronary Syndrome without ST-Segment Elevation. N Engl J Med. 2001 Vol. 345, No. 7
- Effects of pretreatment with clopidogrel and aspirin followed by long-term therapy in patients undergoing percutaneous coronary intervention: the PCI-CURE study. 2001; 358: 527–33.
- Wiviott SD, et al. Prasugrel versus Clopidogrel in Patients with Acute Coronary Syndromes. N Engl J Med. 2007;357:2001-15.
- Zhu B, et al. The onset of inhibition of platelet aggregation with prasugrel compared with clopidogrel loading doses using gatekeeping analysis of integrated clinical pharmacology data. J Cardiovasc Pharmacol. 2011; Mar;57(3):317-324.
- Wallentin L, et al. Ticagrelor versus Clopidogrel in Patients with Acute Coronary Syndromes. N Eng J Med. 2009;361:1045-57.
- Montalescot G, et al. Pretreatment with Prasugrel in Non-ST-Segment Elevation Acute Coronary Syndrome. N Eng J Med. 2013;369:999-1010.
- Davierwala PM, et al. Does Timing of Coronary Artery Bypass Surgery Affect Early and Long-Term Outcomes in Patients With Non–ST-Segment–Elevation Myocardial Infarction? Circulation. 2015;132:731-740.
- Deeik RK, et al. Appropriate timing of elective coronary artery bypass graft surgery following acute myocardial infarction. Am J Surg. 1998;176:581–585.
- Levine GN, et al. Utilization of catheterization and revascularization procedures in patients with non-ST segment elevation acute coronary syndrome over the last decade. Catheter Cardiovasc Interv. 2005;66:149–157.
- Parikh SV, et al. CRUSADE and ACTION Registry-GWTG Participants. Timing of in-hospital coronary artery bypass graft surgery for non-ST-segment elevation myocardial infarction patients results from the National Cardiovascular Data Registry ACTION Registry-GWTG (Acute Coronary Treatment and Intervention Outcomes Network Registry-Get With The Guidelines). JACC Cardiovasc Interv. 2010;3:419–427.
- Brilinta® [package insert]. San Francisco, CA: AstraZeneca; 2009
- Hansson EC, Jidéus L, Åberg B, et al. Coronary artery bypass grafting–related bleeding complications in patients treated with ticagrelor or clopidogrel: a nationwide study. Eur Heart J. 2016;37(2):189-197.
- Gherli, et al. Safety of Preoperative Use of Ticagrelor With or Without Aspirin Compared With Aspirin Alone in Patients With Acute Coronary Syndromes Undergoing Coronary Artery Bypass Grafting. JAMA Cardiology. 2016 Nov 1;1(8):921-928.
- 2014 AHA/ACC Guideline for Management of Patients with Non-ST-Segment Elevation Acute Coronary Syndromes. JACC. 64, 24, 2014.
Share this post:
